Cortisol: The Stress Hormone and Its Impact on Your Health
Cortisol, often called the stress hormone, plays a vital role in health. Learn about its functions, the dangers of imbalance, and effective strategies to manage chronic stress and improve your well-being.
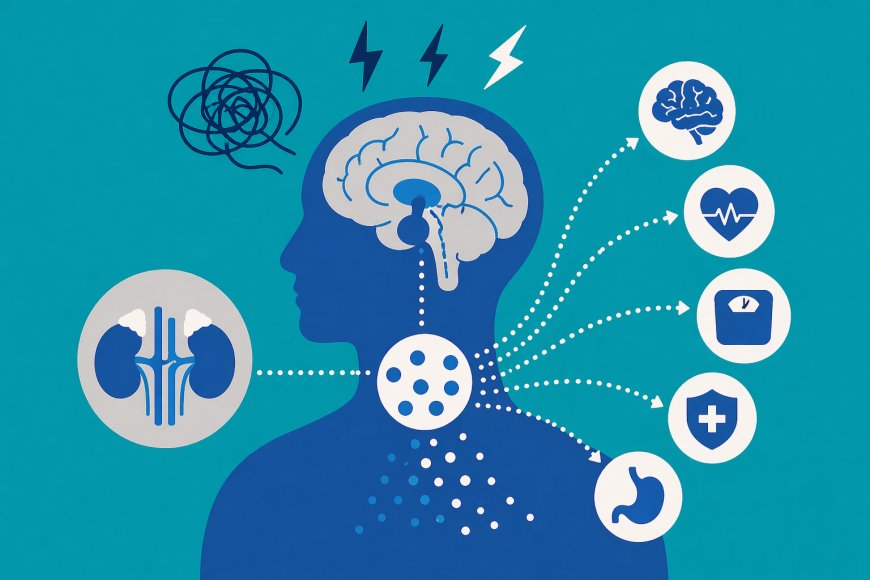
Deep within every bodily response to stress, a silent regulator operates with precision, managing energy, reprioritizing physiological systems, and preparing the body for survival. Cortisol is often misunderstood, sometimes blamed for obesity, anxiety, or depression, yet its reality is far more complex. It is not merely a stress hormone but a central orchestrator linking the brain, endocrine system, and behavior.
What Cortisol Is and Why It Matters
Cortisol belongs to the glucocorticoid family and is secreted from the adrenal cortex. It operates within a highly regulated system known as the Hypothalamic-Pituitary-Adrenal axis, a network that connects the brain to hormonal responses.
Its role extends beyond acute stress. It regulates sleep-wake cycles, blood glucose, immune responses, and inflammation. What makes cortisol unique is its dual nature: essential for maintaining internal balance, yet potentially harmful when chronically elevated or suppressed.
The Regulatory System: How Cortisol Is Controlled
Cortisol secretion follows a tightly controlled biological system. Stress signals begin in the hypothalamus, which releases CRH, stimulating the pituitary gland to release ACTH, which in turn activates the adrenal glands to produce cortisol.
This system is governed by a negative feedback loop that maintains balance. Once cortisol rises, it signals the brain to reduce further production.
Cortisol also follows a circadian rhythm. It peaks in the early morning to activate the body and gradually declines throughout the day. Disruptions in sleep, lifestyle, or chronic stress disturb this rhythm, leading to systemic imbalance.
Physiological Functions: A Multi-System Hormone
Cortisol influences nearly every system in the body.
In metabolism, it mobilizes energy by breaking down proteins and fats while increasing glucose production. This ensures that vital organs, especially the brain, receive sufficient energy during stress. However, chronic activation leads to muscle loss, high blood sugar, and fat redistribution.
In the immune system, cortisol suppresses inflammation and immune responses. While this is beneficial in acute situations, prolonged elevation weakens immunity and increases susceptibility to infection.
In the cardiovascular system, cortisol enhances vascular responsiveness and helps maintain blood pressure and fluid balance. Deficiency, as seen in adrenal disorders, can lead to dangerous drops in blood pressure.
In the brain, cortisol affects cognition, mood, and emotional regulation. Acute exposure sharpens focus, but chronic exposure damages memory-related structures and amplifies fear responses, contributing to anxiety and depression.
Cortisol Imbalance: When Regulation Fails
Cortisol operates within a precise range. When this balance is disrupted, two major conditions emerge.
Excess cortisol, or hypercortisolism, may result from internal disorders such as tumors or from prolonged use of corticosteroid medications. It leads to metabolic dysfunction, weight gain, hypertension, weakened immunity, and psychological disturbances.
Deficiency, or hypocortisolism, often seen in adrenal insufficiency, leads to fatigue, low blood pressure, weight loss, and poor stress tolerance. In severe cases, it can escalate into a life-threatening crisis.
Beyond these clinical conditions, there exists a functional imbalance linked to chronic stress, where cortisol rhythms become irregular without clear disease. This state manifests through fatigue, sleep disruption, anxiety, and cognitive impairment.
Chronic Stress: The Turning Point
Cortisol is designed for short-term survival responses. When stress becomes chronic, the system shifts from adaptation to dysfunction.
The brain begins to treat everyday psychological stress as a biological threat, leading to repeated activation of the HPA axis. Over time, cortisol secretion becomes dysregulated, presenting as sustained elevation, depletion, or irregular fluctuation.
This disruption affects multiple systems simultaneously. In the brain, it impairs memory and increases fear sensitivity. In the immune system, it leads to chronic inflammation despite initial suppression. In metabolism, it drives insulin resistance and visceral fat accumulation. In the cardiovascular system, it increases long-term risk for hypertension and atherosclerosis.
Cortisol also interferes with other hormonal systems, including reproductive hormones and growth regulation, further amplifying systemic imbalance.
Measuring Cortisol: Precision Matters
Assessing cortisol is complex because of its variability and sensitivity to context.
Blood tests provide baseline levels, typically measured in the morning. Salivary tests offer insight into free cortisol and are useful for tracking daily rhythms. Urinary measurements reflect total daily secretion, while hair analysis provides a long-term view of chronic exposure.
Timing is critical. Morning levels reflect peak secretion, while nighttime measurements help detect abnormal patterns. Interpretation must always consider external factors such as stress, sleep, medications, and overall health.
Why Individuals Respond Differently
Cortisol does not act uniformly across the body. Its effects depend on receptor distribution and sensitivity within tissues.
Glucocorticoid receptors mediate most metabolic and immune effects, while mineralocorticoid receptors influence fluid balance and blood pressure. Variations in receptor density, genetic differences, and early life experiences all shape how individuals respond to cortisol.
This explains why two individuals with similar cortisol levels may experience entirely different outcomes, from metabolic changes to psychological responses.
Emerging Scientific Insights
Recent research has reshaped the understanding of cortisol.
Studies have linked disrupted cortisol rhythms to emotional eating and obesity through altered brain activity. Large-scale analyses have shown distinct cortisol patterns across psychological disorders, including depression and post-traumatic stress disorder.
Other research highlights how enzymes regulating cortisol activation in tissues contribute to both metabolic and psychological conditions. Sleep studies demonstrate a strong connection between disrupted sleep, cortisol imbalance, and weight gain, particularly among women.
Advances in precision medicine are now using cortisol profiles to tailor interventions, recognizing that hormonal patterns vary across individuals and require personalized approaches.
Restoring Balance: Beyond Suppression
The goal is not to eliminate cortisol but to restore its natural rhythm.
Medical treatment is necessary in pathological conditions, using hormone replacement or inhibitors under specialist supervision. However, most imbalances are functional and respond to behavioral interventions.
Improving sleep is one of the most powerful regulators of cortisol. Stress reduction techniques such as mindfulness, breathing exercises, and cognitive therapy help recalibrate the HPA axis. Moderate physical activity supports long-term balance, while excessive training may worsen dysregulation.
Nutrition also plays a role. Reducing refined sugars and caffeine, while supporting the body with balanced nutrients and anti-inflammatory compounds, contributes to stability. Social support and psychological safety further reduce chronic activation of stress pathways.
Conclusion: A Hormone of Balance, Not Blame
Cortisol represents a biological paradox. It is essential for survival, yet harmful when persistently activated. It reflects not only physiological processes but also the way individuals interpret and respond to their environment.
Understanding cortisol is not about identifying an enemy within the body. It is about recognizing a system designed for adaptation that becomes overwhelmed when stress becomes constant.
Restoring balance requires addressing the signals that drive cortisol, not suppressing the hormone itself. In doing so, we move closer to understanding the deep connection between mind, body, and environment, and to designing interventions that are both scientifically grounded and human-centered.
What's Your Reaction?