Insulin Resistance: Causes, Symptoms, and Strategies for Prevention
A comprehensive scientific overview of insulin resistance, its causes, clinical indicators, and its profound impact on chronic diseases, fertility, and child health.
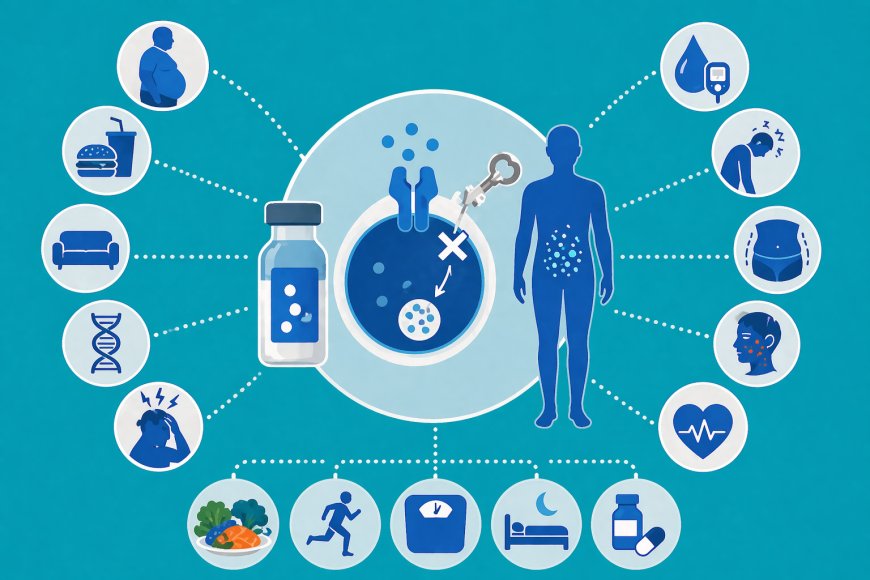
Insulin resistance represents one of the most compelling biological phenomena in the science of endocrinology and metabolism, due to its far-reaching health consequences directly linked to the development of type 2 diabetes, metabolic syndrome, heart disease, and other hormonal disorders. With the term becoming more common in both medical and media spheres, there is a growing need to understand it in a scientifically rigorous manner, free from exaggeration and misleading concepts.
What is Insulin?
Insulin is a protein hormone secreted by the beta cells of the islets of Langerhans within the pancreas. It is the primary biological mediator in regulating blood glucose balance. Insulin is released in response to a rise in blood sugar after eating and enables cells, particularly in the muscles and fat tissue, to absorb glucose for use as an energy source or for storage.
What is the Meaning of Insulin Resistance?
Insulin Resistance is a physiological state in which the body's tissues especially the muscles, liver, and adipose tissue exhibit a diminished response to the effects of insulin. In other words, insulin becomes less effective at stimulating glucose uptake into cells. This prompts the pancreas to produce more insulin in an attempt to compensate for this functional deficit. This compensatory state leads to what is known as chronic hyperinsulinemia, which is itself an independent risk factor associated with a number of chronic diseases, even before the actual development of diabetes.
How Does Resistance Occur at the Cellular Level?
To understand the phenomenon from a cellular perspective:
- Insulin binds to specific receptors on the cell surface.
- This binding activates a series of internal reactions (a signaling cascade) that begins with the phosphorylation of certain proteins, such as IRS (Insulin Receptor Substrate).
- In a normal state, this leads to the activation of glucose transporters (GLUT-4) in muscle and fat cells, allowing for the absorption of glucose.
- In a state of resistance, this chain becomes less efficient, either due to a defect in the number or effectiveness of the receptors, or due to the interference of inflammatory or hormonal signals that affect the transport efficiency of cellular responders.
The Difference Between Insulin Resistance and Type 2 Diabetes
Although the two concepts are related, they are not synonymous:
- Insulin resistance can exist for years without the appearance of diabetes, as long as the pancreas is able to compensate by secreting more insulin.
- Type 2 diabetes arises when the pancreas gradually becomes unable to keep up with this resistance, insulin secretion decreases, and blood glucose levels begin to rise chronically.
The Causes and Factors Leading to Insulin Resistance
To understand insulin resistance as a condition representing a chronic disruption in metabolic balance, it is necessary to trace its roots through two intertwined axes: genetic predisposition on one hand, and the changing lifestyle of the modern era on the other. This condition does not appear suddenly but develops gradually within a network of cellular, environmental, and hormonal interactions.
First: Genetic Factors
Genetic factors play a preliminary role in shaping an individual's susceptibility to insulin resistance. Genetic mutations exist in some individuals that affect insulin receptors or the enzymes regulating the cellular pathways for glucose entry into the cell, such as IRS-1 and PPAR. These mutations do not cause the disease by themselves, but they weaken the efficiency of the response to insulin, especially if they accumulate with contributing environmental factors.
Second: Over-nutrition and Imbalanced Dietary Composition
Diets rich in simple sugars and refined carbohydrates lead to frequent and rapid increases in glucose levels, which necessitates excessive and repeated insulin secretion. This condition exhausts the signaling system within the cell and weakens its sensitivity. Furthermore, saturated and trans fats raise the levels of harmful compounds in cells, such as ceramides, which are fatty molecules that interfere with cellular insulin pathways, particularly at the level of the Akt protein responsible for activating internal glucose transport. This interference contributes to the deactivation of insulin receptors and the loss of response to it.
Conversely, a lack of dietary fiber and good quality protein leads to a decline in satiety, a rapid increase in sugar absorption, and a decrease in muscle mass, which is the largest consumer of glucose in the body.
Third: Obesity and Fat Distribution Within Organs
Visceral obesity, the accumulation of fat within the internal organs, plays a dangerous role in promoting insulin resistance. The impact is not limited to weight alone but also to the location of fat distribution. When fat infiltrates the liver, muscles, and pancreas, it triggers subtle inflammatory reactions that negatively affect the sensitivity of these tissues to insulin. Visceral fat cells also secrete inflammatory cytokines such as TNF and IL-6, which are molecules that contribute to inhibiting the insulin signaling pathway within cells. This process is known as low-grade chronic inflammation and is one of the most prominent causes of metabolic imbalance in individuals with obesity.
Fourth: Lack of Physical Activity
Physical inactivity leads to a reduction in the number of GLUT-4 glucose transporters in the muscles and a decrease in the sensitivity of these tissues to insulin. In contrast, regular physical activity activates a key enzyme known as AMPK, which contributes to improving glucose transport within cells, activating metabolism, and stimulating mitochondria production, thereby naturally enhancing the physiological response to insulin.
Fifth: Sleep Disruption
Chronic sleep deprivation or fragmented sleep directly affects the secretion of hormones that regulate glucose, most importantly cortisol and satiety hormones. Disruption of the circadian rhythm leads to dysfunctions in the pancreas and a decline in the efficiency of the response of muscle and fat cells to insulin. Furthermore, a disturbed biological clock weakens the energy supply in cells and affects the function of proteins that regulate metabolism. The longer the periods of sleep disruption or changes in nighttime rest, the greater the likelihood of the body entering a cycle of chronic insulin resistance.
Sixth: Inflammatory and Hormonal Factors
In addition to the cytokines secreted from adipose tissue, persistent psychological stress and chronic activation of the cortisol axis contribute to enhancing glucose production by the liver and inhibiting the response of tissues to insulin. This makes individuals suffering from constant stress or unstable psychological conditions more susceptible to a deterioration in metabolic balance.
Clinical and Diagnostic Indicators of Insulin Resistance
Diagnosing insulin resistance poses a clinical challenge, as the condition is often silent in its early stages, without explicit symptoms. However, it causes subtle changes that can be detected through clinical and laboratory indicators, reflecting the dysfunction in the physiological response to glucose.
Primary Clinical Indicators
- Increased Waist Circumference: Indicates the accumulation of visceral fat, which is a stronger predictor of resistance than body mass index.
- Acanthosis Nigricans: Darkening of the skin, especially on the neck and under the armpits, which is a sign of chronic hyperinsulinemia.
- Drowsiness After Meals: Indicates a disruption in glucose absorption and insulin responses.
- Difficulty Losing Weight Despite Calorie Reduction: Suggests a disruption in basal metabolism.
Laboratory Indicators
- HOMA-IR (Homeostatic Model Assessment for Insulin Resistance): Calculated from the relationship between fasting blood glucose and fasting insulin levels. An elevated value indicates the presence of resistance.
- Fasting Insulin Level: An elevated level while glucose remains within the normal range may be the first compensatory sign.
- Oral Glucose Tolerance Test (OGTT): Shows the body's response after drinking a glucose solution, with glucose and insulin measured at intervals.
- HbA1c (Glycated Hemoglobin): Does not detect resistance early but helps monitor the transition towards diabetes.
- Triglycerides and HDL Cholesterol: High triglycerides and low HDL are considered indirect indicators.
- Liver Enzymes: Elevated levels may indicate fat accumulation in the liver, a condition associated with insulin resistance.
Insulin Resistance and Fertility
Increased Incidence of Polycystic Ovary Syndrome in Women
Insulin resistance is a crucial factor in the development of Polycystic Ovary Syndrome (PCOS), which is the most common endocrine disorder in women of reproductive age. High levels of insulin stimulate the ovaries to secrete androgens, leading to ovulatory disorders, irregular menstrual cycles, excess hair growth, and acne. This disorder not only hinders pregnancy but also increases the likelihood of miscarriage in the early stages, due to a disturbed hormonal environment.
Decreased Fertility in Men
Insulin resistance affects the pituitary-gonadal axis in men, leading to a decrease in testosterone levels, reduced sexual function, and a decline in sperm quality in terms of count, motility, and morphology. This effect is not limited to the hormonal aspect but reflects a general deterioration in male metabolic balance.
Disrupted Hormonal Balance
The relationship between insulin resistance and reproductive hormones is reciprocal. Just as hyperinsulinemia disrupts hormonal balance, a decrease in estrogen or testosterone levels, in turn, leads to a decline in cellular sensitivity to insulin. This interplay deepens the imbalance and transforms the hormonal dysfunction into a chronic, interconnected condition where it is difficult to separate causes from effects.
Improved Fertility with Improved Insulin Sensitivity
Clinical practice has proven that improving lifestyle through weight reduction, increased physical activity, and better quality of food contributes to restoring hormonal balance and enhancing fertility. Medications like metformin have shown efficacy in stimulating ovulation in women with PCOS. Similarly, increasing muscle mass in men reorganizes testosterone secretion and improves the efficiency of the reproductive system.
Infertility as an Early Indicator of Metabolic Dysfunction
Insulin resistance is not a disorder isolated from the rest of the body's functions; it can be understood as a hidden root of many unexplained cases of infertility. Therefore, the evaluation of insulin resistance should be included early in fertility examinations, not as a secondary symptom, but as a primary factor in explaining reproductive dysfunctions in both sexes.
Insulin Resistance in Children and Adolescents The Silent Danger in Early Growth
Insulin resistance has long been associated in the public mind with adults, especially those who are obese or lead a sedentary lifestyle. However, the medical reality today points to an alarming shift: insulin resistance is now being diagnosed in children and adolescents at increasing rates. This warns of an acceleration of metabolic disorders at an early age and threatens the future public health of coming generations.
The Rising Prevalence in a Young Age Group
Multiple epidemiological studies indicate that childhood obesity especially abdominal obesity is strongly associated with increased rates of insulin resistance. Laboratory tests confirm that children with a high body mass index show elevated levels of fasting insulin, even if they do not exhibit clear pathological symptoms. This prevalence is due to multiple factors: the modern diet, decreased physical activity, and increased exposure to refined sugar and processed foods.
Impact on Growth and Puberty
Insulin resistance affects the hormonal axis of growth and can lead to a disruption in the timing of puberty, whether by abnormal acceleration in females or delay in males. In some cases, it is also associated with the appearance of excess hair in girls and menstrual irregularities, which is an early indicator of broader disorders like Polycystic Ovary Syndrome.
Silent Signs in Examinations
A child or adolescent may not complain of direct symptoms, but some indicators warrant early attention, such as:
- Increased waist circumference relative to height
- Darkening of the skin behind the neck or under the armpits
- Drowsiness after eating, or a frequent craving for sweets
- Lab results showing an unexplained rise in fasting insulin or triglycerides
Future Risks if Neglected
Leaving insulin resistance untreated at this age paves the way for:
- The development of type 2 diabetes at an early age
- Hypertension in adolescence
- Liver dysfunction and the onset of early fatty liver disease
- Mood and concentration disorders, and poor academic performance
The Importance of Early Intervention
The positive news is that the response to lifestyle improvement in this age group is high and effective. In most cases, insulin resistance can be reversed in its early stages through:
- Reducing artificial sugar and sweetened beverages
- Involving children in continuous sports activities
- Regulating sleep and reducing exposure to electronic devices before bedtime
- Involving the family in changing the food environment and entertainment patterns
Therapeutic and Preventive Strategies for Insulin Resistance
Insulin resistance, though reversible in its early stages, becomes a gateway to interconnected chronic diseases if left unaddressed. Therefore, treatment should not be seen merely as correcting glucose levels, but as a strategic plan to rebalance metabolism, restore tissue response, and build a biological defense against the gradual decline of health. This strategy begins with precise behavioral modifications and may extend, as needed, to pharmacological intervention.
Nutrition From Quantity to Quality
The first step in treatment begins with understanding that the quality of food is no less important than its quantity. A low-glycemic index diet helps reduce the peak of insulin secretion and promotes glucose stability.
- Reducing rapidly absorbed carbohydrates such as white sugar, juices, and pastries
- Increasing the proportion of dietary fiber such as legumes, whole grains, and vegetables
- Incorporating good quality protein with every meal to stabilize the glucose response
- Choosing healthy fats such as omega-3, olive oil, and raw nuts while avoiding hydrogenated and saturated fats
Physical Activity The Greatest Variable
Skeletal muscles are the largest reservoir and consumer of glucose. The greater the muscle mass, the greater the body's sensitivity to insulin.
- Resistance exercises such as weight training stimulate the formation of glucose transporters
- Aerobic exercises such as brisk walking, swimming, and cycling increase metabolic efficiency and reduce visceral fat
- Consistency is more important than intensity
Sufficient Sleep
- Sleep for 7 to 9 hours per night
- Establish a fixed sleep and wake time
- Avoid blue light and screens for two hours before sleep
Reducing Stress and Building Psychological Resilience
Chronic stress leads to a constant disruption in the adrenal-pituitary axis, which increases insulin resistance by raising cortisol.
- Deep breathing, meditation, and walking in nature
- Avoiding toxic psychological triggers
Pharmacological Intervention Only When Necessary
When behavioral modifications fail to lower biological markers, medication may be a temporary necessity:
- Metformin
- GLP-1 agonists
- SGLT2 inhibitors
Best Nutritional Supplements That May Help Reduce Insulin Resistance
- Magnesium
- Omega-3
- Chromium Picolinate
- Inositol
- Alpha-Lipoic Acid
- Vitamin D
- Probiotics
Important Note
These supplements are not to be used as a standalone treatment and do not replace dietary modifications, exercise, and sleep regulation. It is also necessary to consult a doctor or a nutrition specialist before using them, especially in cases of children, pregnant women, or those with chronic diseases.
It has become clear through this article that insulin resistance cannot be reduced to a simple rise in sugar or a transient disturbance in hormonal response. Rather, it is a complex pathological structure that affects the body at the cellular, hormonal, neurological, and reproductive levels. It is a condition that is silent in its appearance but devastating in its consequences if not addressed with a holistic approach that integrates diet, movement, sleep, and psychological balance. The real challenge lies not in drug therapy alone, but in redesigning daily behavior to reflect a deep-rooted biological awareness. In another sense, confronting insulin resistance is a confrontation with lifestyle itself, and with our repeated choices that either build us up or slowly tear us down.
What's Your Reaction?