Beyond the Scale: The Hidden Dangers of Weight Loss Drugs
An in-depth look at the unexpected side effects of modern weight loss injections, focusing on the dangerous loss of muscle mass and its long-term health consequences.
In the midst of an accelerating rush of pharmacological discoveries for the treatment of obesity, hormonal injections have emerged as revolutionary solutions for weight reduction, driven by precise physiological mechanisms and formidable marketing. However, this therapeutic advance raises fundamental scientific questions about the nature of what we truly lose during weight loss. Is success to be measured solely by the number of kilograms shed, or must we look deeper into the composition of this lost weight? In this discourse, we delve into dimensions that have been left incomplete in the public debate: muscle mass, aging, hormonal balance, and the biological sustainability of therapeutic outcomes.
The Dawn of the Pharmacological Revolution in Weight Management
The biological revolution in the sciences of metabolism and endocrinology has yielded astonishing progress in drugs aimed at treating obesity. The most prominent outcome has been the emergence of a class of medications now considered a strategic turning point in long-term therapeutic intervention. These drugs, belonging to various categories of hormonal agonists and regulatory peptides, have redefined the limits of clinical efficacy and sparked a broad scientific and economic debate about the future of metabolic medicine.
At the forefront of this class is semaglutide, marketed globally under several trade names, most notably Wegovy for obesity and Ozempic for type 2 diabetes, in addition to the oral medication Rybelsus. It works by stimulating GLP-1 receptors in a way that reduces hunger, slows gastric emptying, and improves blood sugar control, making its effect twofold on eating behavior and metabolic regulation.
Liraglutide, known commercially as Saxenda for weight management and Victoza in the context of diabetes, is the physiological predecessor to semaglutide, with a key difference being the need for daily rather than weekly injections. The drug shares the same mechanism of action on GLP-1 receptors but has a lesser overall effect on weight loss, which has positioned it as a transitional player in the therapeutic evolutionary path.
The third and most ambitious player in this series is tirzepatide, launched as Zepbound for obesity and Mounjaro for diabetes. It features a unique formulation based on dual agonism of GLP-1 and GIP receptors, allowing for a more complex effect on the neural and digestive pathways related to appetite and glucose regulation. This structural synergy in its physiological action has made the drug one of the fastest growing treatments in terms of market share and usage.
In parallel, the market is witnessing the rise of hybrid therapeutic combinations like CagriSema, which combines semaglutide with the hormone cagrilintide to enhance satiety and regulate energy storage. Additionally, the drug Amycretin is advancing as a new experimental mixture of GLP-1 agonists and the hormone amylin, offering a tri faceted effect in controlling food intake, sugar, and fat.
Parallel drug pathways have also evolved away from the appetite axis, most notably the drug bimagrumab, which acts as an inhibitor of the Activin II receptor to block the effect of myostatin and stimulate muscle tissue growth. This opens a new avenue for reducing fat without weakening the muscular structure. However, this approach is still in the clinical trial phase and has not yet reached widespread use.
The Economic Weight of These Medications
Evaluating these drugs is no longer possible in isolation from analyzing their sweeping economic impacts. Recent estimates indicate that the global market for injectable obesity drugs exceeded 26 billion dollars in 2024. Predictive models suggest this figure will multiply to over 400 billion dollars by 2034, in what is considered one of the fastest growing pharmaceutical sectors in modern history.
Semaglutide is the cornerstone of this financial expansion, with sales nearing 28 billion dollars in a single year and expectations to surpass the 90 billion mark in less than a decade. Tirzepatide, for its part, recorded profits exceeding five billion dollars in its first year, with estimates pointing to more than 18 billion dollars in the following year. These indicators confirm that the competition between major pharmaceutical companies, such as Novo Nordisk and Eli Lilly, is no longer merely technical or medical but has also become a financial and strategic battle.
The Proliferation of These Drugs
This economic growth has been reflected in the widespread use of injectable drugs at both the therapeutic and social levels. The number of semaglutide prescriptions in the United States has risen to more than 13 million annually, while tirzepatide prescriptions in the UK jumped from 3,000 to over a million in just one year. British health authorities estimate that about 3.4 million people are eligible for Mounjaro, with plans to distribute 220,000 prescriptions through the public health sector by 2028, while the actual number of users in the private market is estimated at over 1.5 million.
This expansion has not been without its cultural and psychological effects. A shift in users dietary consumption patterns has been observed, with a decline in sales of some high calorie food items, indicating societal behavior changes driven by these drugs. Some experts even classify these drugs as pressure factors on traditional food systems and health economics.
The Biological Mechanisms of Injectable Drugs in Weight Loss
Understanding the Regulatory Pathways of Obesity
Obesity is not merely the result of fat accumulation but a reflection of a complex structural imbalance in the body's energy regulation. This imbalance arises from an interplay of genetic, behavioral, and environmental factors. Obesity drugs do not directly burn fat as commonly believed. Instead, they reprogram hormonal signaling pathways that regulate appetite, insulin response, and energy balance.
GLP 1 and Its Effect on the Brain
Many of these drugs are based on stimulating the GLP 1 receptor, a peptide naturally secreted after meals. It enhances insulin secretion, reduces glucagon, slows gastric emptying, and most importantly signals satiety to the brain. Drugs like semaglutide artificially prolong this signal, leading to reduced appetite and calorie intake.
GIP and Its Dual Effect
Tirzepatide stimulates both GLP 1 and GIP receptors. This dual activation improves insulin sensitivity, enhances satiety, and amplifies metabolic regulation beyond single pathway drugs.
Amylin as a Third Dimension
Amylin contributes to appetite suppression and delayed gastric emptying. Combining GLP 1 with amylin analogues creates a multi layered regulatory effect on eating behavior and metabolic balance.
Indirect Effects
Although these drugs do not directly break down fat, the calorie deficit they create forces the body to utilize fat stores, leading to reductions in visceral fat and waist circumference.
What Are We Actually Losing
What Happens When the Body Loses More Than It Should
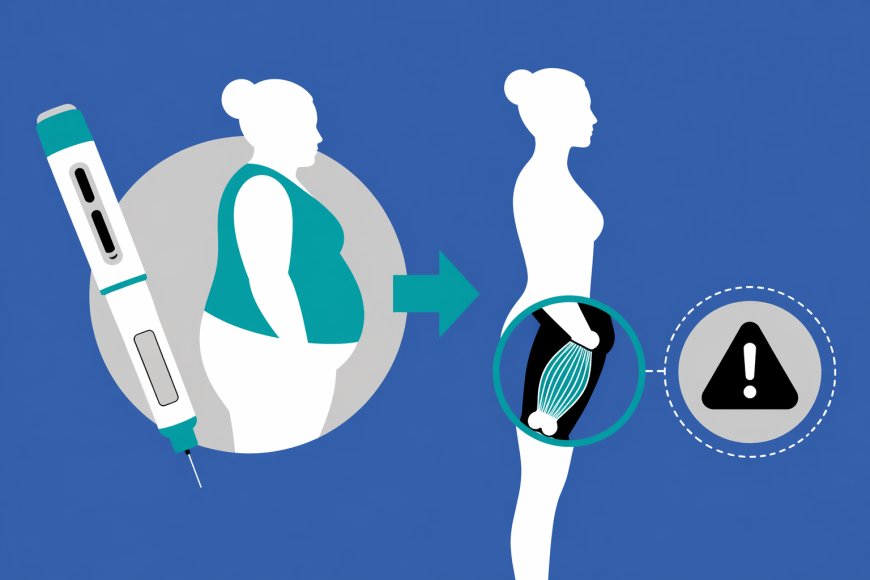
Weight loss is not only about fat reduction. It involves changes in body composition, including lean mass such as muscle. Clinical evidence shows that 30 to 40 percent of weight lost through GLP 1 based drugs may come from muscle mass.
The BELIEVE Study
In a key study, semaglutide alone resulted in significant weight loss, but a considerable portion was muscle. In contrast, bimagrumab preserved muscle mass, while combination therapy showed improved fat loss with reduced muscle loss.
Why Muscle Loss Occurs
Muscle loss is linked to reduced caloric and protein intake combined with low physical activity. These drugs do not directly support muscle preservation, leading to breakdown of muscle protein during energy deficit.
Clinical Implications
Loss of muscle reduces metabolic rate, increases risk of weight regain, weakens insulin sensitivity, and raises the risk of frailty and falls, especially in older populations.
Impact on Metabolism
Muscle is the primary driver of basal metabolic rate. Losing it reduces calorie burning efficiency and increases susceptibility to metabolic disorders.
Impact on Aging
Muscle mass is a key indicator of biological age. Its decline accelerates aging, reduces mobility, and weakens hormonal and immune balance.
Impact on Body Integrity
Muscle supports structural stability, movement, and resilience. Its loss reduces the body's ability to withstand stress, illness, and recovery demands.
In Conclusion
Obesity requires a therapeutic approach that considers body composition, not just weight. While injectable drugs represent a major advancement in reducing fat mass, they simultaneously introduce risks related to muscle loss, metabolic decline, and long term functional weakness.
What's Your Reaction?